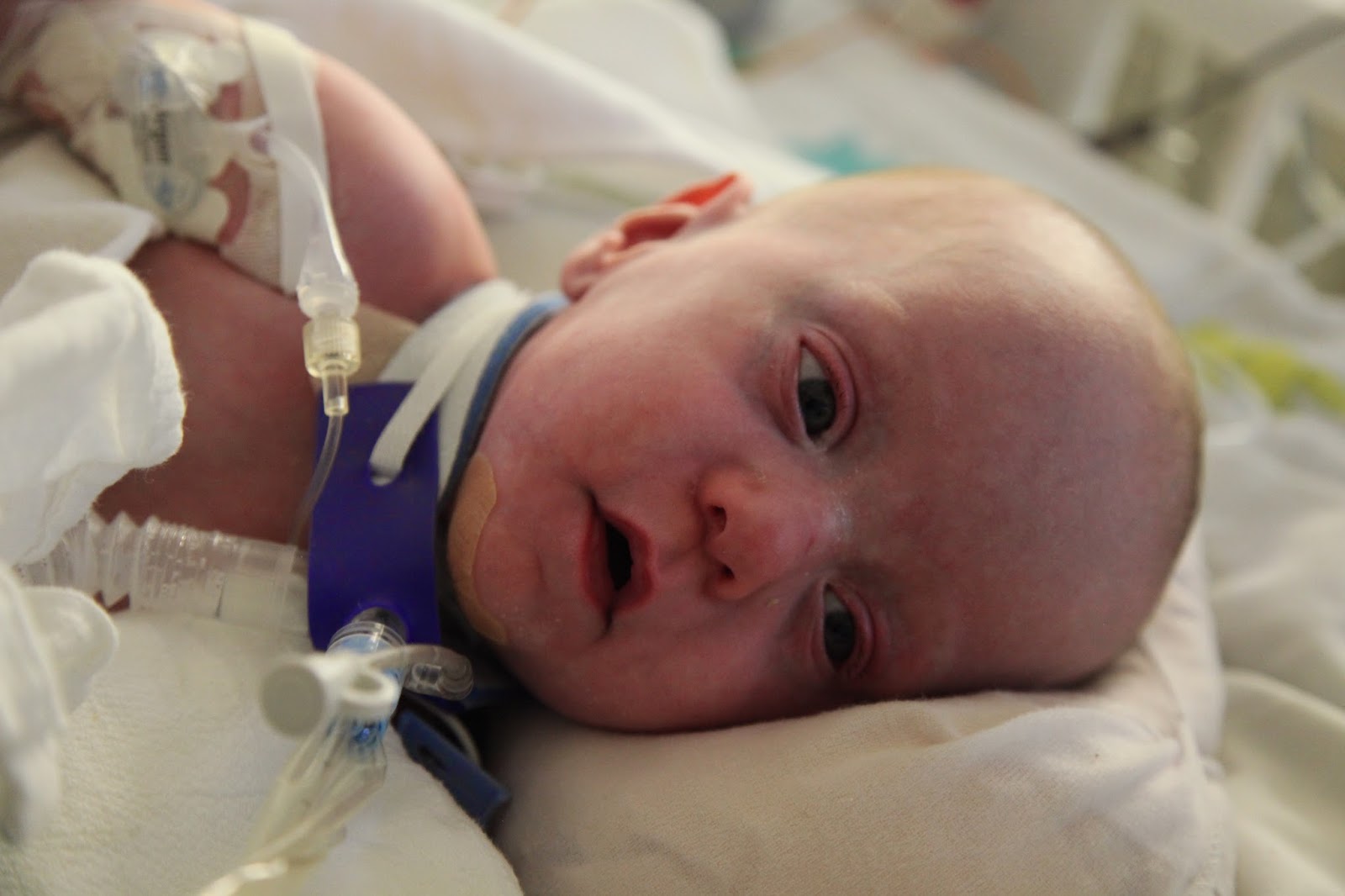
Roscoe has been staying awake longer and longer each day, which is great for us to see because we get glimpses of the "old" Roscoe returning. One of the nurses tried using Tylenol to make him more comfortable, rather than using a heavier drug he's been on (called midozolam). It let him remain more awake, so when one of the nurses came to talk with him he flashed a few of the smiles that we're so familiar with:
I love this boy. I love him when he smiles, when he sleeps, when he cries, and when he just stares with no expression as if to say "Will you hold me?".
Monday, June 30, 2014
Pulmonary Hypertension Clarification
We spoke with Dr. Fineman last night with a few follow-up questions about the two roads ahead of us. He informed us that if we choose surgery and it was successful, Roscoe will be started on the special drug called remodulin (which I mentioned in a prior blog post). Since the drug is relatively new, it can only be administered by a trained nurse, which means that Roscoe would stay at UCSF through the remainder of his recovery until he was ready to go home. With his severe chronic lung disease, this could be several months.
Dr. Fineman also clarified a little about Roscoe's pulmonary hypertension. He said that Roscoe actually has two forms of pulmonary hypertension. First, he has hypertension in the pulmonary arteries that go from his heart to his lungs, due to his chronic lung disease. He has this pulmonary hypertension on both sides. Second, he has hypertension in the pulmonary veins that go back from his lungs to his heart, due to pulmonary vein stenosis. He only has this pulmonary hypertension on the left side, because that is the side with the narrowed veins. The surgery would repair (either temporarily or long-term) the hypertension in his pulmonary veins. The aggressive treatments with remodulin and bosentan would hopefully repair the hypertension in his pulmonary arteries.
Dr. Fineman also clarified a little about Roscoe's pulmonary hypertension. He said that Roscoe actually has two forms of pulmonary hypertension. First, he has hypertension in the pulmonary arteries that go from his heart to his lungs, due to his chronic lung disease. He has this pulmonary hypertension on both sides. Second, he has hypertension in the pulmonary veins that go back from his lungs to his heart, due to pulmonary vein stenosis. He only has this pulmonary hypertension on the left side, because that is the side with the narrowed veins. The surgery would repair (either temporarily or long-term) the hypertension in his pulmonary veins. The aggressive treatments with remodulin and bosentan would hopefully repair the hypertension in his pulmonary arteries.
Ronald McDonald House
A few days ago, Alisha and I got a room at the Ronald McDonald House here in San Francisco. When we arrived we put our names onto the list and luckily a spot opened up, so now we can stay here. The house is a charity organization that provides housing and other resources to families of critically ill children. With this opening, now we are able to stay only a few miles from Roscoe with the comfort of our own space.
In our room (#9) we have a bed, a sink, a small couch, a desk and reliable internet access (which I use to write these blog posts). We share a bathroom with the room next door to us, but haven't hit any conflicts so far. God has provided for us so greatly through this entire process that we haven't had to pay one single hospital bill, pay for a single hotel room, or even pay much for parking or transportation. It is hard to leave my home and live in a strange city for a few months, but if it has to happen then this is the easiest way to do so. God is good and has provided for us in many ways.
In our room (#9) we have a bed, a sink, a small couch, a desk and reliable internet access (which I use to write these blog posts). We share a bathroom with the room next door to us, but haven't hit any conflicts so far. God has provided for us so greatly through this entire process that we haven't had to pay one single hospital bill, pay for a single hotel room, or even pay much for parking or transportation. It is hard to leave my home and live in a strange city for a few months, but if it has to happen then this is the easiest way to do so. God is good and has provided for us in many ways.
Sunday, June 29, 2014
Two Hard Roads
Roscoe's future options will be decided on Tuesday. On Tuesday the doctors involved with Roscoe will meet with the surgeons to determine the viability of surgically repairing Roscoe's pulmonary vein stenosis. This meeting will occur without Alisha and I there. Either way things get decided, we have two hard roads ahead of us.
If the surgeons feel that such a surgery would be too risky to justify the possible outcome, they may deny surgery as an option. Remember that the veins they'd be operating on are 2mm in diameter. The veins are shown in the x-rays below, which were taken during the cardiac catheterization (the catheter is the long, thin tube in the pictures):
Road #1:If the surgeons deny that surgery is an option then we'll have no option (aside from a miracle) to repair Roscoe's pulmonary vein stenosis. Without a possible repair, we'd basically be forced to watch Roscoe wait out his remaining days on a ventilator until no amount of breathing support will keep him alive or until his heart fails from the strain. We'd be able to get rid of all of Roscoe's IVs and probably most of the monitors, so that we could just spend quality time with him. We're not yet sure how much time he'd have, since it would all depend on how much they could get his pulmonary hypertension to stop flaring up. This would be a difficult road to travel, especially knowing that we had no other choice.
Road #2:
If the surgeons agree that surgery is an option, then Alisha and I will have a talk with the pulmonary hypertension team (along with the surgeons) about the probability of various outcomes. The first question would be Roscoe's chances of making it through the surgery alive (his hypertension flare up during the cardiac catheterization causes some doubt). If he did make it through the surgery alive, Roscoe would be hooked up to a life support machine that would keep his heart beating and lungs functioning. They said that he might be on such a machine for up to 3 days, and could also die during that process. If Roscoe survived to that point, he'd need to heal from open heart surgery. Once that happened, his pulmonary vein stenosis would be at least temporarily repaired so they could much more aggressively treat his chronic lung disease with medications that are not possible with his current narrowed pulmonary vein.
If the surgeons feel that such a surgery would be too risky to justify the possible outcome, they may deny surgery as an option. Remember that the veins they'd be operating on are 2mm in diameter. The veins are shown in the x-rays below, which were taken during the cardiac catheterization (the catheter is the long, thin tube in the pictures):
Road #1:If the surgeons deny that surgery is an option then we'll have no option (aside from a miracle) to repair Roscoe's pulmonary vein stenosis. Without a possible repair, we'd basically be forced to watch Roscoe wait out his remaining days on a ventilator until no amount of breathing support will keep him alive or until his heart fails from the strain. We'd be able to get rid of all of Roscoe's IVs and probably most of the monitors, so that we could just spend quality time with him. We're not yet sure how much time he'd have, since it would all depend on how much they could get his pulmonary hypertension to stop flaring up. This would be a difficult road to travel, especially knowing that we had no other choice.
Road #2:
If the surgeons agree that surgery is an option, then Alisha and I will have a talk with the pulmonary hypertension team (along with the surgeons) about the probability of various outcomes. The first question would be Roscoe's chances of making it through the surgery alive (his hypertension flare up during the cardiac catheterization causes some doubt). If he did make it through the surgery alive, Roscoe would be hooked up to a life support machine that would keep his heart beating and lungs functioning. They said that he might be on such a machine for up to 3 days, and could also die during that process. If Roscoe survived to that point, he'd need to heal from open heart surgery. Once that happened, his pulmonary vein stenosis would be at least temporarily repaired so they could much more aggressively treat his chronic lung disease with medications that are not possible with his current narrowed pulmonary vein.
One of the pulmonary hypertension experts drew this picture on a whiteboard to explain the three pathways by which pulmonary hypertension can be medically treated (ie: drugs). To summarize, he showed us how nitric oxide and sildenafil cause the body to dilate blood vessels (good), a newer drug called remodulin also causes the blood vessels to dilate, and how bostentan (which Roscoe is already taking) blocks a chemical that causes blood vessels to constrict. They said that if Roscoe survives the surgery, he will be started on remodulin in addition to bosentan. The remodulin would be taken subcutaneously, like an insulin pump would be used to treat diabetes. This would be yet another machine that Roscoe would be hooked up to that he could go home on. He'd stay at UCSF while he's started on this new drug. Roscoe would continue to have periodic checkups at UCSF to check for scarring/re-narrowing in his pulmonary veins, most likely for many years to come.
So there you have it. We'll either go down a road where we watch our son slowly fade away, or where he barely survives and gets hooked up to more machines and monitored more heavily. At this point, we don't know which road will be taken but we know it will be hard. The prayerful support from you all gives us the energy to continue down such a road, and hopefully the answer to those prayers from God will bring our son safely home.
Saturday, June 28, 2014
Late Update
Roscoe's day started somewhat rocky as I walked in and he was having a desaturation due to having an arterial IV's dressing changed and having a new IV put into his other hand. If memory serves me correctly, since his trach tube surgery a little less than 3 weeks ago, he's had:
After Roscoe settled down, they attempted to put in another PICC line but the attempt failed. While they attempted the PICC line, I went out walking around the nearby Haight-Ashbury area:
After I got back he was sleeping (due to heavy sedation during the procedure). He slept for a good part of the day, then woke up and had a good remainder of the day as well. He even threw in some smiles for good measure.
Roscoe is still at 100% oxygen (no nitric oxide) until he stabilizes a little more and they're able to wean him off of the breathing support. I'll post an update tomorrow about the plan for his future. It looks like the important doctors' meeting will occur on Tuesday, after which his fate will be agreed upon (including us in the decision-making).
Head: 2 IVs, 1 PICC attempt
Right Arm: 2 IVs, 1 PICC
Left Arm: 2 IVs
Right Leg: 2 IVs, 2 PICC attempts
Left Leg: 1 IV, 1 PICC attempt
Feet: Too many pin pricks to count
After I got back he was sleeping (due to heavy sedation during the procedure). He slept for a good part of the day, then woke up and had a good remainder of the day as well. He even threw in some smiles for good measure.
Roscoe is still at 100% oxygen (no nitric oxide) until he stabilizes a little more and they're able to wean him off of the breathing support. I'll post an update tomorrow about the plan for his future. It looks like the important doctors' meeting will occur on Tuesday, after which his fate will be agreed upon (including us in the decision-making).
Baby Einstein
With Roscoe waking up from sedatives but unable to be held, we've had to figure out some ways to keep his mind occupied. We recently purchased a set of "Baby Einstein" DVDs because we knew he'd need some stimulation and there's only so much that we can give him at the bedside before it gets old or before we're worn out. Without the ability to take him outside and show him the wonders of creation, we had to settle for some baby/toddler-oriented visuals from Disney.
Here are videos from the first time he watched them a few days ago. They seemed to really catch his interest, without over-stimulating him. The movements were slow, the sounds were dull, and there was minimal flashing/movement.
We hope that these shows will assist Roscoe's development by introducing him to colors, sounds, numbers, shapes, and concepts that he wouldn't encounter until later on.
Friday, June 27, 2014
A Day of Healing
Although Roscoe's recovery is something to talk about, it isn't the biggest news in San Francisco this weekend. As luck would have it, Alisha and I will be in San Francisco attending to Roscoe while other parts of the city attend the gay pride parade and associated events around town. We are guessing that the influx of people this weekend will negatively effect our commute time, but give us some colorful scenery.
Since our commute to the hospital runs directly through the Castro district, we figure we'll get our fair share of visuals this weekend, even though we won't be at the parade itself. Our conversation recently went something like this:
Alisha: "How many naked people do you think we will see this weekend?"
Shaun: "It depends what you mean by 'naked'. Like fully naked with nothing on, probably 5."
Alisha: "Yeah, I was going to guess 4."
Shaun: "If you mean partial nudity, then probably lots."
I thought it especially hilarious that our commute took us directly past the following street in the Castro:
What the hospital room feels like
We share some cute baby videos and pictures and then descriptions of new machines or procedures that have come to Roscoe, but for the most part the hospital room just feels like this all day:
There is constant beeping from his heart monitor (upper left) and a periodic shrill blast of air from his ventilator (on the right). When Alisha and I aren't on our phones or attending to him, this is basically what we do in the hospital room. Our eyes glance up at the monitors, then back at Roscoe, then over at another monitor, then back at Roscoe, etc. I am thankful that he has these monitors, because without them some of his problems would have gone undetected or mistreated, however they have a tendency to drive us nuts if we don't tune them out.
Just play this video on repeat and you'l know how it feels to be here with us. Then you might need to go out for a walk in the fresh air to clear your head too. Thank you for praying!
There is constant beeping from his heart monitor (upper left) and a periodic shrill blast of air from his ventilator (on the right). When Alisha and I aren't on our phones or attending to him, this is basically what we do in the hospital room. Our eyes glance up at the monitors, then back at Roscoe, then over at another monitor, then back at Roscoe, etc. I am thankful that he has these monitors, because without them some of his problems would have gone undetected or mistreated, however they have a tendency to drive us nuts if we don't tune them out.
Just play this video on repeat and you'l know how it feels to be here with us. Then you might need to go out for a walk in the fresh air to clear your head too. Thank you for praying!
Songs of Encouragement
For those who follow this blog and may not be connected to our network of friends through facebook, I wanted to post a few links. These links are to gospel songs that were sung in support of Roscoe. Alisha and I have been touched by the prayers that have been worded, artwork that has been crafted, and now songs that have been sung in support of Roscoe.
When the song says "let the weak say I am strong", I think of how Roscoe was barely able to lift his own arms when he was born, but now he can thrash anything put into his hands. When the song says "let the poor say I am rich", I think of how impoverished Alisha and I would be if all of these medical bills came to us (by now he has most likely crossed the $3 million mark). We still have not been asked to pay one medical bill, rent one hotel room, or pay practically any parking fees while caring for Roscoe. When the song says "let the blind say I can see" I think of how when he was born he could barely open his eyes because the lids were fused shut, and now his eyes are so big and bright that they almost seem unmatched to his face.
God has truly blessed Roscoe with growth, and Roscoe wouldn't be here (or be the little man he is today) without God's support and healing. We pray that God will carry out this work to its completion and bring our little boy home, healthy and stable despite the odds against him.
- "Shout to the Lord" by Latina Brooks
- "What the Lord has done in me" by Sephra Scheuber
When the song says "let the weak say I am strong", I think of how Roscoe was barely able to lift his own arms when he was born, but now he can thrash anything put into his hands. When the song says "let the poor say I am rich", I think of how impoverished Alisha and I would be if all of these medical bills came to us (by now he has most likely crossed the $3 million mark). We still have not been asked to pay one medical bill, rent one hotel room, or pay practically any parking fees while caring for Roscoe. When the song says "let the blind say I can see" I think of how when he was born he could barely open his eyes because the lids were fused shut, and now his eyes are so big and bright that they almost seem unmatched to his face.
God has truly blessed Roscoe with growth, and Roscoe wouldn't be here (or be the little man he is today) without God's support and healing. We pray that God will carry out this work to its completion and bring our little boy home, healthy and stable despite the odds against him.
Mostly Bad Results
Roscoe's big day of procedures came to an end with some good news, but mostly bad news. As an overview, he got the lung scan ("perfusion scan") done from 10-10:30am, then the cardiac catheterization from 3:30-7:00pm. They skipped the bronchoscopy because he had some stability problems during the cardiac catheterization (referred to as the "cath" from now on to save on typing). Read below for the detailed results. It looks like we are facing a dangerous surgery as our only option.
We took Roscoe to the perfusion scan room which contained a long x-ray machine which looked similar to a miniature MRI machine. They injected Roscoe with some radioactive material dissolved in saline solution, so that they could trace the radioactive material travelling through his lungs. The tech accidentally spilled a few drops of the solution onto the floor, so he had to check all of our shoes with a Geiger counter before we left. The scan of Roscoe's lungs only lasted 1-2 minutes, but it showed much more circulation going to his right lung (the good one) than to his left (the one with pulmonary vein stenosis). I only saw the picture, so when they schedule a family meeting to go over the details we'll hopefully find out how abnormal his flow was.
Roscoe getting transferred from his crib to the machine
Roscoe in the machine getting scanned by x-rays
The on-screen output showing the circulation through his left and right lungs (bottom two small patches) and his brain (faded upper patch). The top image is from one side and the bottom image is from the opposite.
Viewing Roscoe through the center of the scanning machine
The Geiger counter they used to scan for radioactive material on the floor
Roscoe returned to his room and played a little before the cardiac cath. Each passing day he has grown more alert, so it was great to see the old Roscoe start returning. Before he went to the cath lab, they moderately sedated him for transport. Once we arrived at the cath lab (which we first visited back in February) they gave us an overview of the process, got him settled, and then gave us a pager to let us know when the procedure was progressing.
Transferring Roscoe from his crib to the cath lab table
Cath lab equipment, looks super high-tech
Dr. Moore holding Roscoe's pacifier as he explained the cath process to us
While the procedure was happening, we drove to Fisherman's Wharf to get fish & chips and pizza for an early dinner, since normally we wouldn't be able to travel that far. They paged us right as we finished, so we headed back and waited anxiously for the results. They let us know that they'd foregone the bronchoscopy, but didn't say why over the phone.
Dr. Moore met us in the hallway to explain the results of the cardiac cath. Going into the procedure, he expected to see similar results to the first cath he'd done in February, where with one of Roscoe's two left pulmonary veins exhibiting stenosis (narrowing). When he did the cath, he found that both of Roscoe's left pulmonary veins were now exhibiting stenosis. Not only that, but the stenosis had gone from mild/moderate in February to moderate/severe in June. He attributed this to Roscoe's body growing at a rate that was faster than these pulmonary veins. This observed data puts a time limit on Roscoe's ability to survive in his current state, because eventually he will reach a point where his right lung will cease to circulate blood back to the heart (which will cause all sorts of issues, most likely heart failure).
To put numbers on it, the diameter of Roscoe's left pulmonary veins as they enter his heart are both roughly 2mm, when they should be 2.5mm (upper) and 5-6mm (lower). This means that his set of pulmonary veins is only able to deliver about 50% of the blood flow that it should be delivering. It also causes a pressure differential of up to 5x the normal blood pressure that should be in his lungs (pulmonary hypertension). His heart has to work against that higher pressure, which makes the 5x blood pressure a threat of heart failure. As Roscoe continues to grow bigger, his body's needs for oxygen will increase, but his ability to deliver oxygen will either stay the same or decrease.
Dr. Moore said that right now Roscoe's left pulmonary veins are too small to expand with either a balloon or stent. They have stents that will fit, but since they are so small (a wire mesh tube that's ~1mm in diameter) the stent would have limited expandability and couldn't grow with him to support him long-term. Dr. Moore's opinion that the only option to resolve Roscoe's pulmonary vein stenosis is surgery. He explained that surgery would carry significant immediate risk due to Roscoe's instability (ie: there is a chance Roscoe wouldn't survive the surgery). He also said that even if successful, the surgery only works as a long-term solution 50-60% of the time. The rest of the time, the surgery site grows scar tissue and re-narrows the vein opening. We prayed for the doctors to come to the best solution for Roscoe's long-term health, but right now it feels like we're backed into a corner with no other options to save his life.
Right now you might be asking, "So what's the good news?". The good news is that Roscoe's pulmonary vein and vessels don't seem to be narrowed except where they enter the heart. This is good, because it allows for the surgical option and localized treatment. If the veins or vessels were completely narrowed, Roscoe would have no option for long-term treatment. Also he said on multiple occasions that Roscoe is "tough", which is what he'll need if we move forward with the risky surgery. The last piece of good news is that a few hours after the surgery, Roscoe was active and kicking, despite having been briefly paralyzed a few hours prior. He was smiling even more than usual, which gave us a chance to snap this picture as he laughed with Alisha:
The neonatalogist was concerned about Roscoe's pulmonary hypertension causing heart failure over the next 18-24 hours, because the pulmonary hypertension escalated due to the agitation of the cardiac cath (some escalation was expected, but it went further than they thought). She did say it was a great sign that he came out of the paralysis so quickly and was so alert. The neonatalogist added yet another sensor to Roscoe's arsenal of sensors. This time, it's a forehead strap that measures the oxygenation in his brain. If heart failure occurs and they are unable to get blood pumped through his lungs due to the hypertension, this reading will let them know how long Roscoe's brain will have gone without oxygen (brain damage). For now, it just looks funny:
Now that UCSF has all of this information gathered, they will find a time when Alisha and I can meet with all of the experts involved (Dr. Moore for the catheterization, Dr. Fineman for the pulmonary hypertension, Dr. Cohen for surgery) along with their teams to discuss the data and risks of surgery or other treatments (of which I'm not sure there are any). Hopefully this meeting will occur sometime on Friday. Once UCSF arranges the meeting, Alisha and I will know more about the risk level of Roscoe having open heart surgery (90% survival vs 50% survival vs 10% survival), how bad his current state is if we choose to avoid surgery, and any other questions that might arise. It looks like we'll be at UCSF for at least another 1-2 weeks, since they'd want Roscoe as calmed and stable as possible if the surgery were to take place.
One final note: Please do not send text messages or phone calls to Alisha. Messages like "We are praying for you" or "How is Roscoe doing?" are just reminders that her baby is in critical condition in the hospital. Since she always has her phone on her, messages which might be intended as encouraging actually just remind her of the scary situation we're in (when she might be out on a walk, trying to clear her head). She is under a considerable amount of strain having to process all of this removed from the comfort of her home. If you feel like texting/calling, you can try my phone but I most likely won't answer. :)
We tried to implement some stress relief by constructing our own ice cream sandwich from two cookies and ice cream in the UCSF cafeteria
Thursday, June 26, 2014
Happy Baby
Yesterday, Roscoe had a good day of stability. Along with that stability came more of the Roscoe that we're used to seeing, with his big, attentive eyes and curiosity for his hands. Below are some pictures we took when he was alert and playing, despite being on sedatives. As the husband of a photographer, I must warn you that the pictures were taken in low light (so we didn't annoy Roscoe's comfortable state), so they are more grainy than they would have been in full light. There, you have been warned.
We also took a video while he played with his hand, to show that he hasn't lost his curiosity even when he's got a constant feed of sedatives:
We won't post the results of his procedures until the end of today (most likely very late at night), so hopefully until then this gives you a good reminder of the little boy you've been praying for these many months.
The Big Day (take #2)
Today, Roscoe will have 3 procedures done:
- Ventilation scan
- Cardiac Catheterization
- Bronchoscopy
The ventilation scan is just to give extra information before going into the cardiac catheterization. The bronchoscopy is a visual inspection of his airway to make sure it has good integrity and function. The bronchoscopy will be done opportunistically, since he'll already be heavily sedated by an anesthesiologist (try scoring that word when playing scrabble or hangman!). The major procedure of the day is the cardiac catheterization.
The cardiac catheterization will mainly be an exploratory surgery, with possible interventions taken to repair his pulmonary vein stenosis. The procedure will feed a tube through his leg artery, into the right atrium of his heart (labeled as "RA" below), through to his left atrium (labeled as "LA" below), and then into the pulmonary vein which has narrowed (shown darkened on the middle left below):
As mentioned in some previous blog posts, Dr. Moore and his team will first perform some exploratory measurements to see how effectively the oxygenated blood is received from Roscoe's lungs through his pulmonary vein. They will also measure the effectiveness of various treatments for chronic lung disease (such as nitric oxide, sildenafil, and maybe some other drugs).
After the measurements are performed, Dr. Moore will consult with his team and determine (based upon their collective experience) what will be the proper treatment for Roscoe's pulmonary vein stenosis. The first option will be to place a small balloon inside the narrowed vein, inflate the ballon, then deflate the balloon and see if the vein stays open. If that doesn't work, then the next option would be to place a stent (expandable rigid mesh tube) inside the narrowed vein. They would use the balloon to increase the diameter of the stent, then leave the stent in place in Roscoe's heart. Eventually, Roscoe's vein would grow new tissue and bind itself to the stent (making it very difficult to remove). There are various types of stents that the team will have on hand, and they will choose the most appropriate type based upon what they find during the exploratory phase of the procedure.
The last option will be surgery, if the prior two options fail. We've heard varying opinions, but it seems like the surgery is only appropriate once kids are at least a few years old, and even then it is very risky (since they need to stop both the heart and blood flow to the heart).
Our hope is that God will grant these doctors wisdom to choose what will give Roscoe the best possible outcome (and with God, all things are possible). If the doctors are able to repair Roscoe's pulmonary vein stenosis, then it will make his chronic lung disease (his other major issue) much easier to treat, since it will open up more common options for treatment. Please pray fervently with us that Roscoe's results are fantastic and that this is finally the start to the healing we have been longing for.
Wednesday, June 25, 2014
Prepped for Tomorrow
Roscoe's big day will come tomorrow, when he'll have a lung scan, cardiac catheterization, and bronchoscopy. After these 3 procedures, we'll have a great deal more information about Roscoe's current state and any possible solutions or paths that Roscoe might use venture toward good health.
Today he had another good day of progress. They were able to totally wean him from nitric oxide (for the second time), keep his breathing rate at 35 breaths/minute, lower the base pressure (PEEP) from 5 to 6 as I mentioned in the previous blog post. Throughout the day he remained stable with overall fewer drops in his oxygen saturation and less irritability. We snapped a few pictures throughout the day to show him at various stages of rest. It's funny because nowhere outside of a hospital would you see a baby sleeping in a position that looks like its lost in the laundry pile. Hopefully this means Roscoe will be good at playing hide-and-seek:
The nurses also positioned him on his stomach, which is how he typically slept before the trach tube surgery. We could tell he loved it because his saturations stayed high and he slept for a long stretch of time with no additional sedatives needed to keep him resting:
Today he had another good day of progress. They were able to totally wean him from nitric oxide (for the second time), keep his breathing rate at 35 breaths/minute, lower the base pressure (PEEP) from 5 to 6 as I mentioned in the previous blog post. Throughout the day he remained stable with overall fewer drops in his oxygen saturation and less irritability. We snapped a few pictures throughout the day to show him at various stages of rest. It's funny because nowhere outside of a hospital would you see a baby sleeping in a position that looks like its lost in the laundry pile. Hopefully this means Roscoe will be good at playing hide-and-seek:
The nurses also positioned him on his stomach, which is how he typically slept before the trach tube surgery. We could tell he loved it because his saturations stayed high and he slept for a long stretch of time with no additional sedatives needed to keep him resting:
In case you were curious, the bandage on the back of his head is to cover the salve that's being applied to the last remnant of his bedsore that he developed a little under 2 weeks ago. Hopefully it will be completely healed within a few days and he'll be able to once again lie flat on his back.
In an earlier post, I also forgot to include a picture of his trach supplies which hang in his room:
The green bag and pink box contain any dressings and straps that would be needed to replace his trach tube. The clear bag taped to the wall (labeled "Obturator") is a piece that goes down the middle of a trach tube to add stiffness, for situations like when it's being inserted into his neck. In the lowest pockets of the green bag there is a replacement trach tube in the right-hand pocket. The right-hand pocket contains an emergency trach tube which is one size smaller, in case the trach hole starts healing up and gets too small.
Oxygen 67%, Nitric Oxide 2.5ppm
Roscoe had another night and morning of mild progress. His oxygen was weaned from 70% to 67%, his nitric oxide was weaned from 10ppm to 2.5ppm, and his base breathing support pressure was weaned from 6 to 5 (which will make the breathing support easier on his lungs). Here's a video we took yesterday with him resting, which is how we see him most of the time now:
Although Roscoe isn't back to the level of stability he had on Saturday when he was at 50% oxygen, the pulmonary hypertension team has tentatively scheduled him for the cardiac catheterization tomorrow. He will have a big day tomorrow if all goes as planned, because in the morning he'll start out with his lung scan, then move to the cardiac catheterization, then possibly get a bronchoscopy too (to check for airway obstructions or other issues).
Although Roscoe isn't back to the level of stability he had on Saturday when he was at 50% oxygen, the pulmonary hypertension team has tentatively scheduled him for the cardiac catheterization tomorrow. He will have a big day tomorrow if all goes as planned, because in the morning he'll start out with his lung scan, then move to the cardiac catheterization, then possibly get a bronchoscopy too (to check for airway obstructions or other issues).
Comforting Words
Roscoe is on heavy sedatives which are gradually being decreased. His heart rate remains high due to his pulmonary hypertension, but also because he is being given albuterol (an inhalant that improves lung function) and diuretics (to get rid of excess fluids). Both the albuterol and diuretics have the potential to raise his heart rate. He will look normal and comfortable, but when he is awake his heart rate got into the 180-190 range if he was even mildly active. When he is in a deep sleep his heart rate will be 160, when previously it hovered around 90-100 in deep slumber.
To combat the high heart rate, Alisha and I will read books to him. Though he is sleeping, we know that he hears our voice and it comforts him. The pictures below are of Alisha reading him a book to get him to settle down and to remind him that she's still there, even though he can't see her:
I am proud of Alisha for undergoing such a tumultuous time and still being brave enough to remain positive for Roscoe's benefit, and still having faith in God when immediate healing hasn't been granted (though we've asked time and time again).
To combat the high heart rate, Alisha and I will read books to him. Though he is sleeping, we know that he hears our voice and it comforts him. The pictures below are of Alisha reading him a book to get him to settle down and to remind him that she's still there, even though he can't see her:
I am proud of Alisha for undergoing such a tumultuous time and still being brave enough to remain positive for Roscoe's benefit, and still having faith in God when immediate healing hasn't been granted (though we've asked time and time again).
Midnight Update
Not much to update with, but for those who were curious I thought I'd post an update. When we left the hospital tonight Roscoe's oxygen was still at 70%, but his nitric oxide had been lowered to 10ppm and his breathing support rate was lowered to 35. When we get in tomorrow we'll see if he's taken any steps forward or backwards through the night. We hope to post an update around noon tomorrow, but the hospital wireless internet access is very unreliable, so often we are unable to post an update even if we have the time to write it.
Tuesday, June 24, 2014
Cards of Support
Roscoe got some fun cards delivered to him from the Stiles children who attend the Sebastapol congregation. Jonah, Lily, and Micah made cards for Roscoe and had their dad deliver them when he met me for lunch a few days ago. We liked the creativity they showed, and I especially appreciate the unexpected formality of the card on the left which closes with "Signed, Jonah" (he is around 8 years old).
It encourages us to know that people are praying for Roscoe, but it is especially touching when children pray for him. There is something about children praying for other children that's so innocent. We have heard from parents all over the country who say their children will constantly remind them to include Roscoe in their prayers. Thank you all for training your children to consider the less fortunate and support others through prayer, Roscoe will someday grow to appreciate the compassion that his peers have shown for him.
Mild Improvement
Since we arrived he has stayed somewhat steady at 70% oxygen, with his oxygenation staying in the low 90's. It looks like we are on a road of extremely slow progress back towards his baseline. Alisha and I are starting to identify nurses which we like and those we don't, based mainly on how quickly they react to Roscoe's ups and downs. It is a comforting thing to be able to leave him with a nurse that we trust. When Roscoe has a nurse that doesn't react very quickly then it troubles us to leave him alone for fear that she will fail to give him the support/care that he needs when he needs it.
PS: I apologize for the late update, the wireless internet access here at UCSF has been pretty horrible today.
Monday, June 23, 2014
Still Unstable
I know that lots of people are checking the blog, so I wanted to post an update before we went to sleep tonight. Roscoe's condition hasn't gotten worse, but it also hasn't gotten any better. He is still on 100% oxygen and 20ppm of nitric oxide to maintain his oxygen saturation at normal levels. His sedation has been increased as well to keep him calm.
Since the last update, Roscoe started receiving albuterol and some other inhalant to dilate both his breathing passageways and the blood vessels in his lungs. These additional measures have seemed to help, because now his saturation goes into the 96-99 range, rather than 90-94. The doctors haven't yet had to give Roscoe a paralytic drug, even when they re-set his arterial IV and adjusted his PICC line depth today. Mostly when we look at him he is very sleepy and calm, even when his heart rate is high.
Alisha and I will head to Amy and Ricardo's house for the night and will then come back in the morning and post another update (probably around noon). We appreciate your prayerful support through this (again) stressful time.
Since the last update, Roscoe started receiving albuterol and some other inhalant to dilate both his breathing passageways and the blood vessels in his lungs. These additional measures have seemed to help, because now his saturation goes into the 96-99 range, rather than 90-94. The doctors haven't yet had to give Roscoe a paralytic drug, even when they re-set his arterial IV and adjusted his PICC line depth today. Mostly when we look at him he is very sleepy and calm, even when his heart rate is high.
Alisha and I will head to Amy and Ricardo's house for the night and will then come back in the morning and post another update (probably around noon). We appreciate your prayerful support through this (again) stressful time.
Procedures Cancelled
The two procedures that Roscoe was scheduled to undergo today have
been cancelled, due to Roscoe's instability. After I wrote the blog post last
night, Roscoe had a big episode where had to be manually ventilated (ie:
"bagged") and his oxygen saturation dropped into the 30's. As a
result, the doctors increased his sedation and painkillers by 10% and put him
back on a full 20ppm of nitric oxide. They did this because any time Roscoe
wakes up now, his heart rate shoots up into the 170-180 range even if he
visually looks calm. Last night we were reading a book to him shortly before
the episode occurred:
Roscoe's stability was progressing nicely until roughly 2 days ago. After they put in the new PICC line, inserted an arterial line (to monitor blood pressure and make blood samples less intrusive), and started weaning him from nitric oxide his condition seemed to worsen. Now the doctors are trying to back-track to undo whatever happened to cause this degradation in his health. The pulmonary hypertension specialists were very disappointed to hear this, because they had hoped to do the cardiac catheterization today to narrow in on a long-term solution for Roscoe's issues. They want to perform the procedure when Roscoe is at his "baseline" (ie: normal behavior and stability) so today certainly isn't the day for that. Today Roscoe will regularly desaturate into the 80's when he get significant cares or if he wakes up too much. It is sad for us to look at his rolling eyes and see our little boy trapped inside this sedated body. We can tell that he hears us and that he wants to look around, but the sedation is restraining his curiosity. The spirit is willing, but the flesh is weak.
At this point they aren't sure whether the episodes are pulmonary hypertension or if they are a worsening of his chronic lung disease. They plan to take more measurements from blood samples to check how stressed his heart is, which will hopefully determine whether they should treat the pulmonary hypertension or the chronic lung disease. Both are inter-related, but the doctors are just trying to figure out which they will tackle as the primary issue that's hurting his health.
We will post updates as they occur later today. Right now the primary goal is to stabilize Roscoe back to the level he was at 2 days ago before this downturn began. For Alisha and I, it is very discomforting (downright scary) to see his numbers, sedation, and instability all coming back to the levels they were at two weekends ago when he nearly left us. There is even a plan for one dose of paralytics later today as they change his trach straps and re-set the arterial line. The paralytics bring back bad memories for me, so I am not looking forward to it.
Sunday, June 22, 2014
The Big Day
Monday will be one of the most important days in Roscoe's young life. On Monday, Roscoe will undergo two procedures:
On Sunday, Roscoe took another step backwards. His breathing support started the day at around 60% oxygen and ended the day at 100% oxygen. Along with his increase in breathing support, his heart has also started beating very fast. For instance, just now he calmly woke up and his heart rate jumped to 170 (when normally it would be around 130). His heart rate and oxygen requirements are most likely related, as his heart would need to beat faster if his body isn't getting enough oxygen. These two factors probably indicate that his pulmonary hypertension is triggering again, although not as severely as it was last week. Monday's results will give much needed insight into the current state of his pulmonary hypertension and what can be done to resolve it.
Since Roscoe's heart rate keeps skyrocketing even when he is normally awake, the nurses give him additional sedative and painkillers to keep him calm. Though Alisha and I hate to see it happen, they said that right now we're choosing the lesser of two evils (pulmonary hypertension crisis vs pharmaceuticals). Once the cardiac catheterization happens, they can start making plans to wean the drugs once the pulmonary hypertension has been dealt with. We took two videos of Roscoe in a medically-induced slumber, while he dreamed of wonders and adventures that only his mind knows at this point. You can tell by the expressions on his face that he was experiencing something great, but we don't quite know what it was.
While we'd certainly love for Roscoe to be happy, awake, and vibrant, right now we are stuck between a rock and a hard place. His pulmonary hypertension seemed to be getting worse over the past few days, which is disappointing because he had several days in a row of very positive progress.
We especially ask that you pray for the surgeons and doctors involved in Roscoe's care on Monday. We will post updates when we know the time that Roscoe is scheduled to go through both procedures. Please pray that the surgeons and doctors:
- Ventilation Scan
Roscoe's will undergo a lung scan which will give the doctors get a preview of how well the blood is being distributed throughout his lungs. This preview will assist them by letting them know what they might expect during the cardiac catheterization (his second procedure of the day).
- Cardiac Catheterization
Roscoe will also get a cardiac catheterization, where they thread a small tube from an artery in his leg up through parts of his heart and into the vein that connects his heart to his lungs. As I mentioned in a previous post, the results of the cardiac catheterization will either be to perform surgery at a future date, stent the vein during the catheterization, or to wait for the vein to grow naturally.
My view of the golden gate bridge (with San Francisco in the background)
on my way back from visiting the Sebastapol congregation on Sunday.
on my way back from visiting the Sebastapol congregation on Sunday.
On Sunday, Roscoe took another step backwards. His breathing support started the day at around 60% oxygen and ended the day at 100% oxygen. Along with his increase in breathing support, his heart has also started beating very fast. For instance, just now he calmly woke up and his heart rate jumped to 170 (when normally it would be around 130). His heart rate and oxygen requirements are most likely related, as his heart would need to beat faster if his body isn't getting enough oxygen. These two factors probably indicate that his pulmonary hypertension is triggering again, although not as severely as it was last week. Monday's results will give much needed insight into the current state of his pulmonary hypertension and what can be done to resolve it.
Since Roscoe's heart rate keeps skyrocketing even when he is normally awake, the nurses give him additional sedative and painkillers to keep him calm. Though Alisha and I hate to see it happen, they said that right now we're choosing the lesser of two evils (pulmonary hypertension crisis vs pharmaceuticals). Once the cardiac catheterization happens, they can start making plans to wean the drugs once the pulmonary hypertension has been dealt with. We took two videos of Roscoe in a medically-induced slumber, while he dreamed of wonders and adventures that only his mind knows at this point. You can tell by the expressions on his face that he was experiencing something great, but we don't quite know what it was.
While we'd certainly love for Roscoe to be happy, awake, and vibrant, right now we are stuck between a rock and a hard place. His pulmonary hypertension seemed to be getting worse over the past few days, which is disappointing because he had several days in a row of very positive progress.
We especially ask that you pray for the surgeons and doctors involved in Roscoe's care on Monday. We will post updates when we know the time that Roscoe is scheduled to go through both procedures. Please pray that the surgeons and doctors:
- Have wisdom (in the life decisions they make for Roscoe)
- Have skill (in their ability to carry out the decisions they make)
"Now He was telling them a parable to show that at all times they ought to pray and not lose heart,
...
will not God bring about justice for His elect which cry to Him day and night, and will he delay long over them? I tell you that He will bring about justice for them quickly."
Psalm 23
The last week has been very hard for Alisha and I. We've come to a new realization to what it means to come face-to-face with death and be prepared for it. We have also realized that growing stronger faith comes at a cost of comfort and happiness. Roscoe has shown steady improvements over the past week at Kaiser and now UCSF, but today he hit another rough patch.
The nurses at UCSF were able to completely wean him off of the nitric oxide, when he was at 7ppm yesterday and 15ppm the day before that. This was great news for us. The problem was that there were 2-3 times during the day when Roscoe woke from sleep and could not focus his eyes (they darted back and forth) and was very difficult to console. At first the doctors thought it was withdrawls from the painkiller or sedative (they had tried weaning those by 10% too), so they put the painkiller and sedative back up to the full amount. At one point his heart rate reached the 190's, which it hasn't done in a while. The common response from UCSF when Roscoe's heart rate raised was to give him more painkillers or sedatives, which Alisha and I protested.
A good picture of how we felt today is this:
The picture above is a photo I took of something I stepped on when I stood by his bed today. Rather than it being a gum wrapper or hair clip like you might expect to step on, this is an old IV that was in Roscoe's arm with Roscoe's blood spattered around it on the floor. Not a very comforting sight to see, and today wasn't a very comforting day. While UCSF may have a greater amount of technical expertise, small "oversights" like this are one of the reasons we strongly prefer the treatment at Kaiser.
As I walked around outside to clear my head during a break, Psalm 23 came to mind:
Phrases like "the shadow of death" have new meaning for me, implying that death is so close you can feel it's shadow pouring over your feet. In times when death is that close (like last Saturday), God is still a comfort. A shepherd's rod and staff were used for correcting and training the sheep. Just like that staff, God's word trains us in righteousness so that when rough times come we fall back on it instinctively. Those corrections and training which previously seemed harsh or unnecessary become ultimately valuable when their benefit is seen during periods of trial. Think of how a soldier doesn't appreciate boot camp until he's in the depth of war. Our spiritual correction and training prepares us to be comforted in dark times. When rough times come, we pray. When we are blessed, we give thanks. When Satan tempts us, we choose right.
The nurses at UCSF were able to completely wean him off of the nitric oxide, when he was at 7ppm yesterday and 15ppm the day before that. This was great news for us. The problem was that there were 2-3 times during the day when Roscoe woke from sleep and could not focus his eyes (they darted back and forth) and was very difficult to console. At first the doctors thought it was withdrawls from the painkiller or sedative (they had tried weaning those by 10% too), so they put the painkiller and sedative back up to the full amount. At one point his heart rate reached the 190's, which it hasn't done in a while. The common response from UCSF when Roscoe's heart rate raised was to give him more painkillers or sedatives, which Alisha and I protested.
A good picture of how we felt today is this:
The picture above is a photo I took of something I stepped on when I stood by his bed today. Rather than it being a gum wrapper or hair clip like you might expect to step on, this is an old IV that was in Roscoe's arm with Roscoe's blood spattered around it on the floor. Not a very comforting sight to see, and today wasn't a very comforting day. While UCSF may have a greater amount of technical expertise, small "oversights" like this are one of the reasons we strongly prefer the treatment at Kaiser.
As I walked around outside to clear my head during a break, Psalm 23 came to mind:
The Lord is my shepherd,
I shall not want.
He makes me lie down in green pastures;
He leads me beside quiet waters.
He restores my soul;
He guides me in the paths of righteousness
For His name’s sake.
Even though I walk through the valley of the shadow of death,
I fear no evil, for You are with me;
Your rod and Your staff, they comfort me.
You prepare a table before me in the presence of my enemies;
You have anointed my head with oil;
My cup overflows.
Surely goodness and lovingkindness will follow me all the days of my life,
And I will dwell in the house of the Lord forever.
"All Scripture is inspired by God and profitable for teaching, for reproof, for correction, for training in righteousness; so that the man of God may be adequate, equipped for every good work".
- 2 Timothy 3:16-17
- 2 Timothy 3:16-17
Saturday, June 21, 2014
Wall Art
The hospital has lots of art and decorations on the walls, so once in a while we'll walk by something and it will catch our interest. Some of you may remember the gratitude tree that was painted onto the wall on the 7th floor where Roscoe is housed. We walked by the tree today and it had grown much more full through 5 months of messages of healing. The messages were from parents and from the kids themselves who had been healed:
Early February 2014
Mid June 2014
I was surprised to find our gratitude leaves still on the tree, exactly how we'd left them. The messages we wrote are just as applicable now as they were back then:
Then on the 6th floor I ran across this signed jersey in the Barry Bonds children's wing. It is his signed jersey from the 2007 all-star game. Although I appreciate his generosity, I think this jersey would have been more appropriately hung in the pharmacy.
Like the Back of a VCR
Roscoe is starting to look like the back of a VCR with all of the wires running out of him. Yesterday we got to the hospital a little later than usual. He received a new PICC line in his right arm (which I believe was his 4th) which will be a long-term IV which runs a tube through his artery and near to his heart. If you'd like to see what Alisha's PICC line looked like, click here to see what was outside her arm and here to see the rest of the tube that ran through her veins. The PICC line will be used to deliver Roscoes sedative and painkiller. He also got an arterial IV in his left arm (which was a surprise to us) which they will use to draw blood. This will hopefully prevent further needle pokes and allow his other veins to heal.
With these two new IVs, Roscoe has a total of 3 IVs again (foot, left arm, right arm) along with sensors for CO2, oxygenation, heart rate, breathing rate, and another sensor to measure the fluid content in his system. This is what his room looks like as a whole:
In the upper left is the screen that displays his heart rate (green), blood pressure (red), fluid content (white), breathing rate (yellow) and oxygenation (blue):
Tomorrow we hope to have lots of cute baby pictures (and maybe some videos) to share which will show our little man in his new larger crib. He continues to look better each day, which is very encouraging to us. We are confident that God is watching over Roscoe and giving him this improvement in direct response to the prayers all of you are making.
With these two new IVs, Roscoe has a total of 3 IVs again (foot, left arm, right arm) along with sensors for CO2, oxygenation, heart rate, breathing rate, and another sensor to measure the fluid content in his system. This is what his room looks like as a whole:
In the upper left is the screen that displays his heart rate (green), blood pressure (red), fluid content (white), breathing rate (yellow) and oxygenation (blue):
Below that screen on a small shelf is another machine which monitors his CO2 levels through a sensor attached to his leg. They measure his CO2 because higher levels of CO2 will cause Roscoe's blood vessels to constrict which will increase his blood pressure:
To the right of the screen is a small green screen that controls his continuous feeding (currently at 27mL per hour). Below the screen are two separate pumps that run fluid through his unused IVs to keep them flushed to prevent clogging:
Below Roscoe's bed is a small machine that was injecting potassium into his system to replace any that he lost due to the diuretics he's been taking this past week to keep him from building up fluid in his lungs while he's on nitric oxide.
To the right of Roscoe's bed is the machine that supplies his oxygen at a specified breathing rate and pressure. The top line on the chart you can see a distinction between the breaths that Roscoe is making (smaller) and the breaths that the machine is making (larger):
The output of that machine gets mixed with nitric oxide by another machine further to the right. For those who've read this far, despite the lack of cute baby pictures, you'll be excited to learn that last night his nitric oxide was at 15ppm and Roscoe wasn't stable enough to be weaned to 10ppm. That's exciting because tonight when we left, he was extremely stable at a level of 7ppm:
Subscribe to:
Comments (Atom)